7-year-old male neutered Bassett hound mix
The patient presented to GCVS Internal Medicine Service for evaluation of ascites. He had a history of heartworm disease diagnosed and treated 1 year prior to presentation with melarsomine. Bloodwork (CBC and serum chemistry) from the primary clinic showed mild hyperglycemia and mild hypocholesterolemia. Thoracic radiographs performed at the primary clinic were unavailable for review but were reported to show cardiomegaly.
Grade 2/6 left apical systolic murmur; grade 3/6 right systolic murmur; regular rhythm. Lung sounds clear. Distended abdomen.
Initial visit with Internal Medicine Service
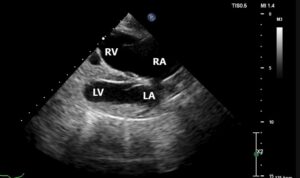
RA=right atrium; RV=right ventricle; LA= left atrium; LV=left ventricle
Recheck with Cardiology Service 2.5 weeks later
Initial visit
Recheck visit with Cardiology 2.5 weeks later
The patient was managed for the next several months after initial presentation with periodic abdominocentesis and medication adjustments to address recurrent right-sided congestive heart failure (CHF). He was switched from furosemide to torsemide after 2 months due to refractory right-sided CHF, and the frequency and/or dose of pimobendan was increased multiple times due to recurrence of ascites. Sotalol was started 5 months after initial presentation due to worsening ventricular arrhythmia. Hydrochlorothiazide was also eventually added due to the continued frequent development of ascites. Additionally, the patient was supportively managed with capromorelin (Entyce) to address hyporexia. Unfortunately the patient presented to the Emergency Service deceased on arrival approximately 6.5 months after initial presentation, presumably from sudden cardiac death.
Trypanosoma cruzi is the protozoan parasite responsible for Chagas disease. Transmission occurs when feces from an infected triatomine insect enter a host through a wound or mucous membranes. Oral consumption of an infected insect is another route of infection. Transplacental and transmammary infection have also been reported in dogs. After infection, the trypomastigote stage of the protozoa will invade the host cells. The myocardium is the primary site of infection in dogs, although other organs can also be affected. The infection eventually results in cell death. Scarring and hypertrophy occur, resulting in arrhythmias, chamber enlargement, and cardiac dysfunction. There are three phases of Chagas disease. There is a rise and fall in the degree of parasitemia in the acute phase. Dogs in this phase may be asymptomatic, although myocarditis and sudden death are possible. In the indeterminate stage, dogs will be seropositive but frequently do not exhibit clinical signs. Some dogs in the indeterminate stage will advance to the chronic phase. The chronic stage is typically when the manifestation of arrhythmias and cardiac dysfunction occur. Chagas disease should be considered in dogs that live in or have visited an endemic area and present with arrhythmias or ventricular eccentric hypertrophy and systolic dysfunction, particularly if the patients are not typical signalment for primary dilated cardiomyopathy (DCM). However, dogs predisposed to the development of primary DCM can also be affected so Chagas disease remains a differential in these patients. One study indicated that dogs with right ventricular enlargement, as in this case, were 3.6 times higher to experience cardiac death1. Unfortunately at this time there are no vaccines or approved specific treatments in the United States for canine T. cruzi infection. The main focus of treatment is addressing complications associated with the disease, including treatment of CHF and arrhythmias. Disease prevention via preventing contact with triatomine insects is also important.